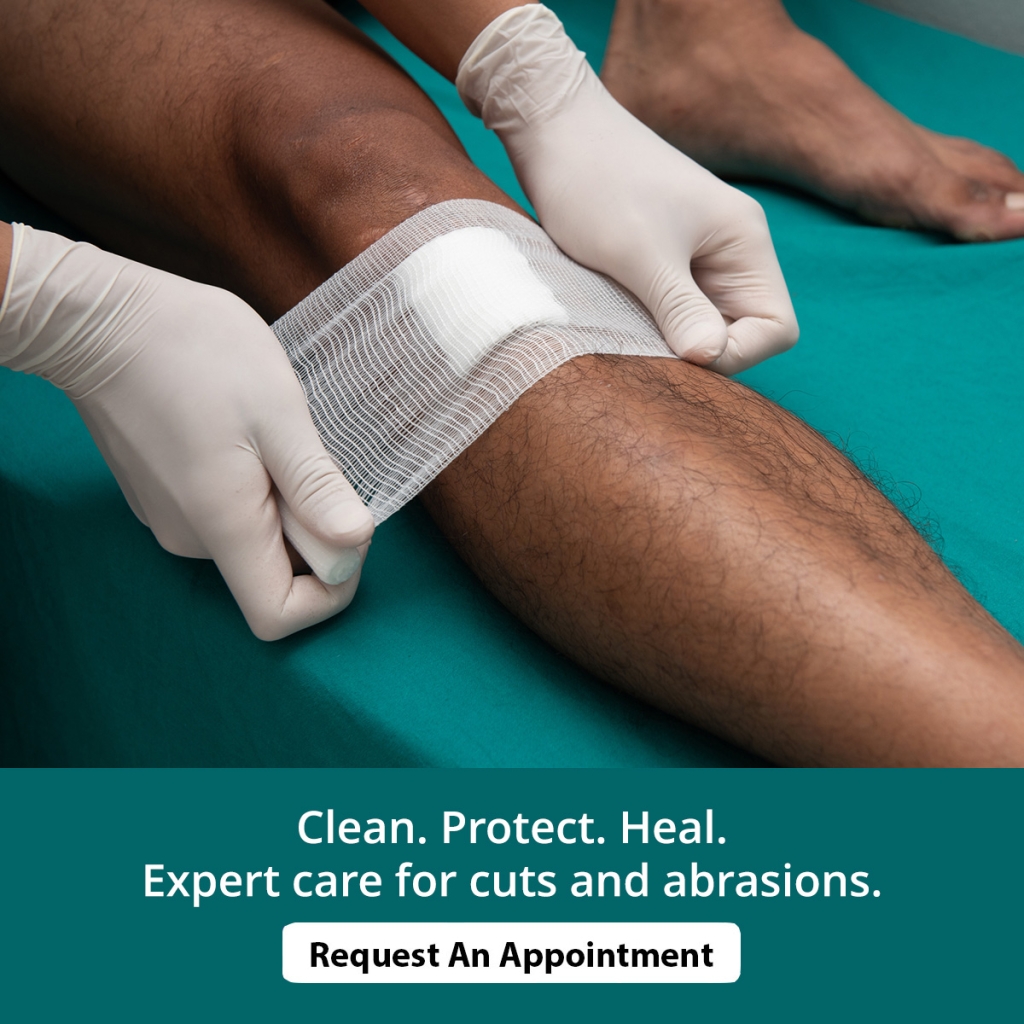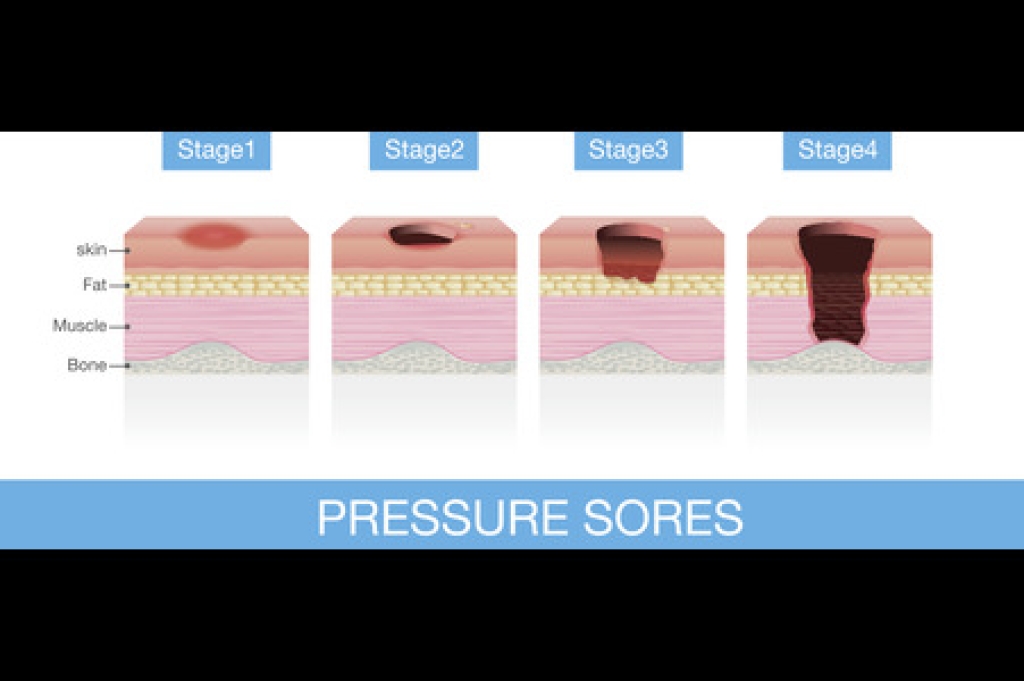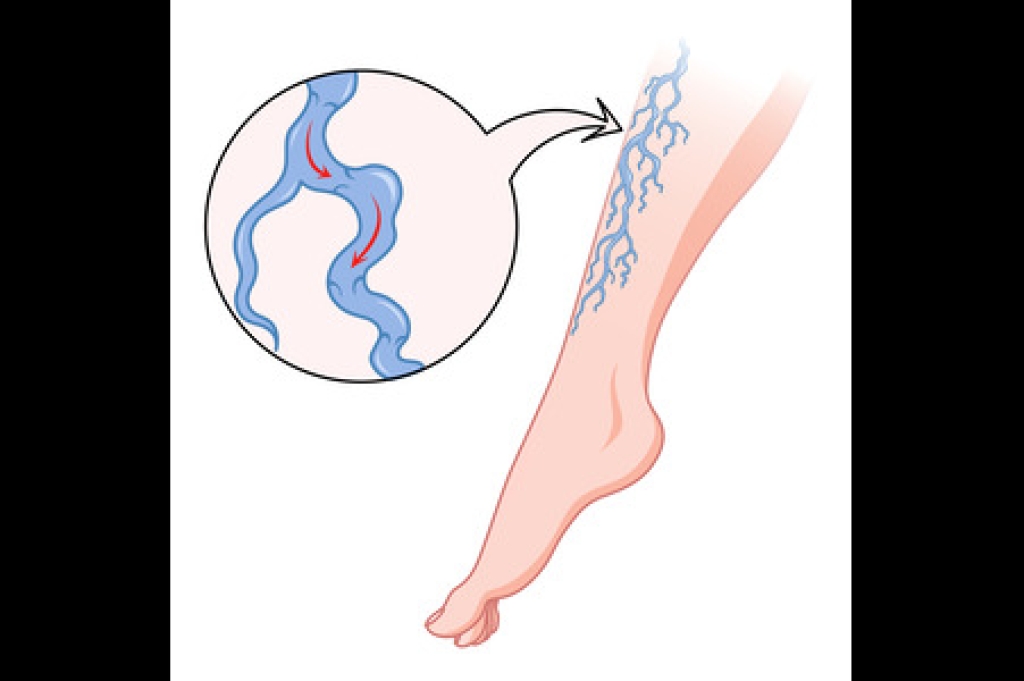
Chronic leg ulcers are wounds on the lower leg that fail to heal within a typical timeframe, often lingering for weeks or months. They usually develop because the skin and underlying tissues are not receiving the support they need to repair themselves. Venous disease is a leading cause, as weakened vein valves allow fluid to pool and increase pressure, eventually breaking down the skin. Arterial problems can also play a role when reduced blood flow limits oxygen and nutrients essential for healing. Diabetes, infections, trauma, and long-standing swelling may further delay recovery or worsen an existing ulcer. These ulcers can be painful, draining, discolored, or surrounded by fragile skin. Without proper treatment, they may return or become infected. Because finding the exact cause is critical for successful healing, it is suggested that you see a wound care specialist for an accurate diagnosis and a personalized treatment approach.
Chronic Wounds and Complications That Slow Recovery
Most wounds follow a predictable healing pattern, but some linger far longer than expected. Chronic wounds are those that fail to progress through normal healing, often remaining open, painful, and vulnerable to infection. On the feet, ankles, and legs, these stubborn wounds can significantly limit mobility and quality of life.
Post-surgical wounds are a common source of concern. While surgery is intended to improve health, the incision site does not always close as planned. Compromised circulation, infection, or pressure can delay healing and leave patients dealing with ongoing discomfort. Professional monitoring and care are essential to ensure the wound is cleaned, dressed, and supported until closure is achieved.
Chronic pain conditions may also complicate recovery. Neuromas, for example, are thickened nerve tissues that can cause persistent pain in the foot. Although not open wounds themselves, they often interfere with normal gait and create pressure points that make the skin more prone to breakdown. Left unaddressed, this discomfort can contribute to recurring sores or prevent existing wounds from closing.
Chronic wounds require specialized attention because traditional home remedies are rarely enough. Advanced wound care techniques may involve debridement, specialized dressings, pressure offloading, or therapies designed to improve blood flow and tissue repair.
If you have a wound on your foot, ankle, or leg that is not healing or continues to reopen, call us today for expert care from our wound specialist.